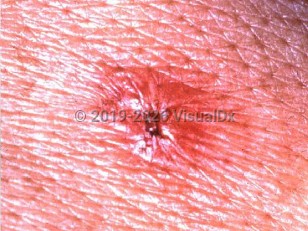
Japanese spotted fever
Alerts and Notices
Important News & Links
Synopsis

First reported in 1984, Japanese spotted fever (JSF) is a tick-borne illness caused by Rickettsia japonica, which is largely limited geographically to Japan's pacific (central and southwestern) coastal regions. Cases have also been reported from the Japanese Sea coastal area along with South Korea and China, and the pathogen has been reported in Taiwan, Thailand, and Laos. The tick vector is Haemaphysalis longicornis. Bites from this species of tick have also been associated with the development of allergy to mammalian meat (see alpha-gal syndrome). Its animal reservoir(s) are still unknown. About 40 cases are reported in Japan each year, and this rickettsia can be of significant pathogenic potential, on par with Rickettsia rickettsii – the agent of Rocky Mountain spotted fever – in older and immunocompromised individuals.
Patients typically present with the triad of fever (100%), a diffuse rash (100%), and an eschar (71%–94%). Other symptoms include myalgias, headache (80%), meningoencephalitis, and, in severe cases, multiorgan failure. Only around a third of patients recall a tick bite. Mortality rate overall is about 2%, but those who present late in illness (6 or more days) have an increased rate for complications including multiorgan failure, disseminated intravascular coagulopathy, and death. Laboratory findings associated with increased severity include elevated WBC, elevated creatine kinase, low platelets, elevated fibrin degradation products (FDP), and elevated C-reactive protein (CRP).
Risk factors for exposure are living in or visiting an endemic area, contact with vegetation including both crops and forested areas (early cases were associated with bamboo shoots), and older age (60-70 years on average).
A seasonal variation in incidence has been noted with most cases presenting during the warmer months of April through November. The presumed incubation period is 7 days, like other rickettsioses; however, it has not been well-defined.
Patients who are older and/or have diabetes mellitus may be at increased risk for severe infections.
Patients typically present with the triad of fever (100%), a diffuse rash (100%), and an eschar (71%–94%). Other symptoms include myalgias, headache (80%), meningoencephalitis, and, in severe cases, multiorgan failure. Only around a third of patients recall a tick bite. Mortality rate overall is about 2%, but those who present late in illness (6 or more days) have an increased rate for complications including multiorgan failure, disseminated intravascular coagulopathy, and death. Laboratory findings associated with increased severity include elevated WBC, elevated creatine kinase, low platelets, elevated fibrin degradation products (FDP), and elevated C-reactive protein (CRP).
Risk factors for exposure are living in or visiting an endemic area, contact with vegetation including both crops and forested areas (early cases were associated with bamboo shoots), and older age (60-70 years on average).
A seasonal variation in incidence has been noted with most cases presenting during the warmer months of April through November. The presumed incubation period is 7 days, like other rickettsioses; however, it has not been well-defined.
Patients who are older and/or have diabetes mellitus may be at increased risk for severe infections.
Codes
ICD10CM:
A77.8 – Other spotted fevers
SNOMEDCT:
186771002 – Spotted fever group rickettsial disease
A77.8 – Other spotted fevers
SNOMEDCT:
186771002 – Spotted fever group rickettsial disease
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:11/20/2022
Last Updated:11/21/2022
Last Updated:11/21/2022
Japanese spotted fever